Pre-2020, few employers meaningfully acknowledged that work and personal lives were inextricably linked. Instead, they sustained “the myth of separate worlds”, as labelled by Harvard Business School’s Professor Rosabeth Moss Kanter, and did not see an employee’s wellbeing as their responsibility.
But, somewhere between the blur of Zoom calls, living room intrusions, hybrid work discussions, lockdown stress, and an increase in family and domestic violence (FDV), the COVID-19 pandemic exacerbated a cultural shift that was already in motion, and the world of work irrevocably changed.
Now, employees want more control, and they want employers to step up.
For many, their health and safety depend on it. For example, if they cannot see a doctor in a medical emergency or cannot access FDV leave when their situation at home has become untenable, their lives can be at risk.
In a powerful message of priorities:
- 91 per cent of 2,000 employees we surveyed in Australia (working a minimum of 20 hours per week, across different industries) thought it was important for their next employer to offer mental wellbeing support; and
- 37 per cent of 1,000 workers surveyed in Australia considered their employer their main source of mental health support.

Why can’t workers access the care they need?
Unfortunately, employees do not have equal access to care.
- A $50 gap payment at the local doctor might be a drop in the ocean to one employee, but to their colleague, it could be the barrier that prevents them from seeking care.
- A five-hour wait at the emergency room may be inconvenient for one employee, but an impossibility for their ill colleague who cannot leave their children alone at night.
- A study in England and Wales found, “People further down the social ladder usually run at least twice the risk of serious illness and premature death than those at the top”.
- A reported80 per cent of men are unlikely to seek help from a phone helpline.
- A psychologist’s appointment can be “especially scarce” in rural and remote communities, and unreliable internet can limit their access to virtual care.
- An FDV victim experiencing coercive control might not have the money, transport, or ‘permission’ to seek care.
Why can’t workers do it alone?
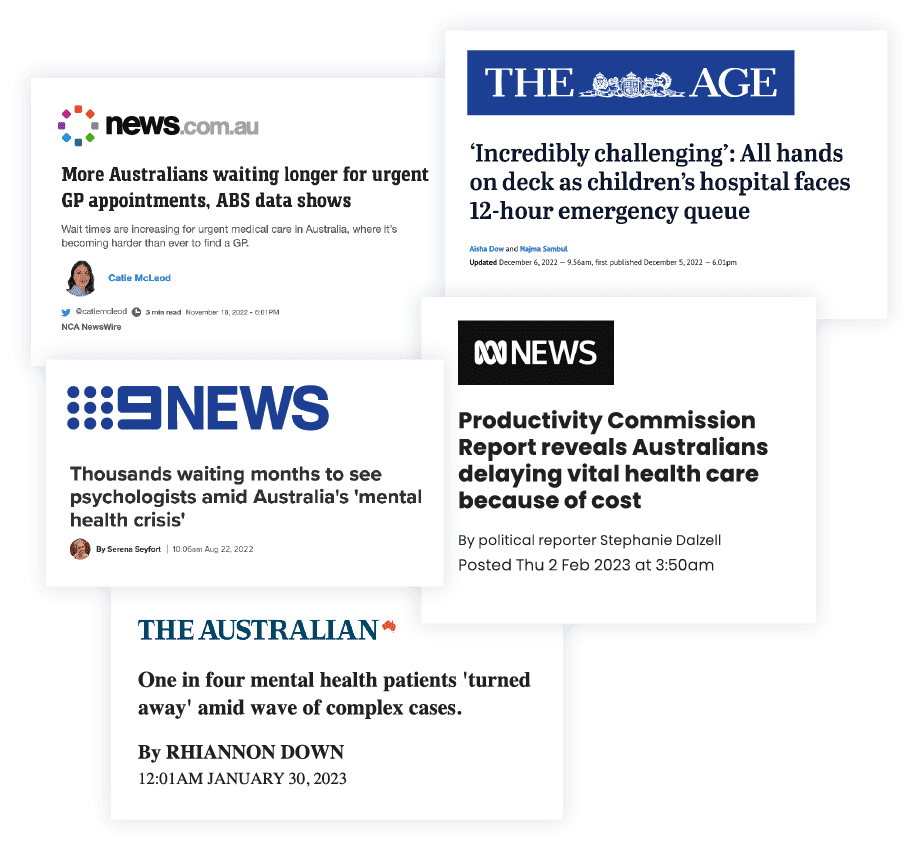
With Australians waiting longer for urgent healthcare appointments, being turned away when their case is too complex, or delaying vital health care because of cost, it’s clear that many workers need help to stay safe and well.
References: The Age, News Limited, Australasian College for Emergency Medicine, Royal Australian College of General Practitioners, Nine News, ABC News, The Australian
“Access block for medical and mental health care is the most pressing issue of our time. More and more members are reaching out to us because they are feeling blocked from accessing care due to cost, or they cannot access quality care within a reasonable amount of time. For the first time in Medicare’s history, the average out-of-pocket cost (gap payment) for a standard GP consult exceeds the Medicare rebate that a patient receives. With the average out-of-pocket charge increasing by 50 per cent over the last decade, people are increasingly looking for alternative ways to access professional medical care.”

Dr Jamie Phillips, MB ChB, AFCHSM, DIMC RCS(Edin), MRCGP(UK), FACRRM(EM), Medical Director, Sonder
What about employee assistance programs (EAPs)?
Traditional employee assistance programs (EAPs) are well-intentioned but suffer a utilisation rate as low as five per cent.
- Not built into the culture;
- Solutions are not the right fit; and
- Poor past experiences.
Interestingly, most EAP offerings exclude the most-needed form of support: medical.
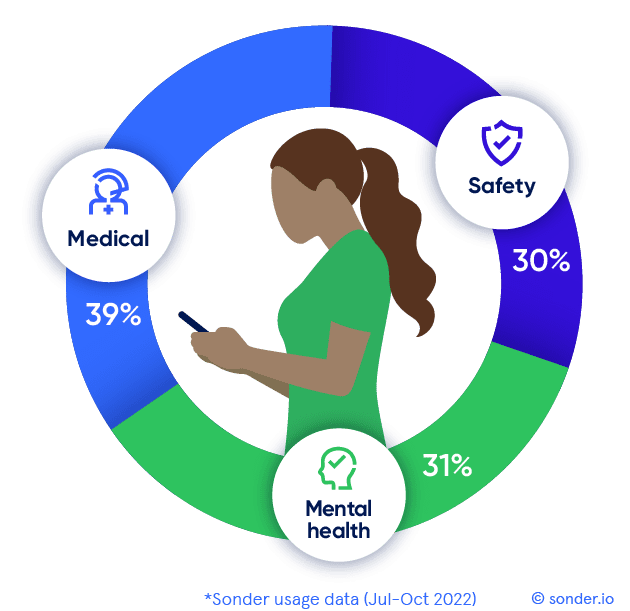
In our sample cohort of 10,000+ people who utilised employer-funded wellbeing support, we found (when we excluded “other/miscellaneous”) that medical support (39 per cent) was required more than either mental health (31 per cent) or safety (30 per cent) support.
And wellbeing is complicated, but most EAP offerings are narrow.
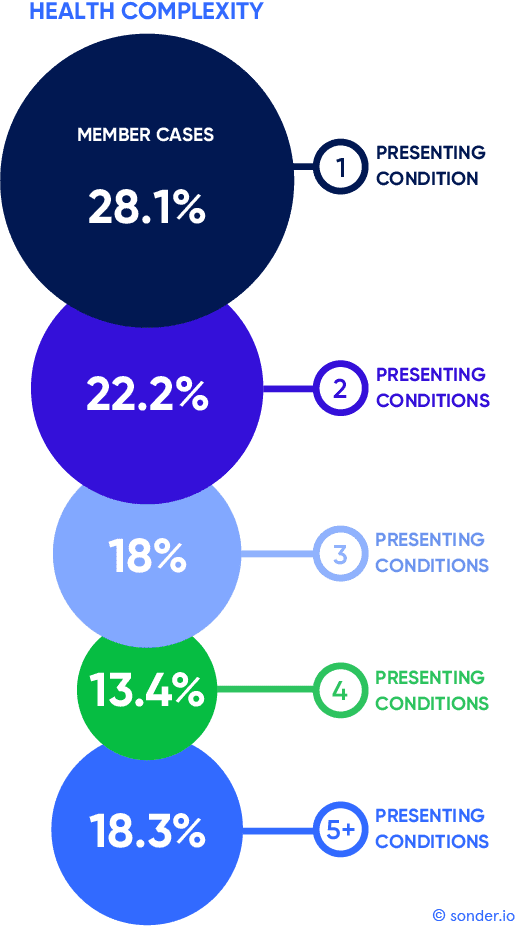
In our sample of 10,000+ member support cases from July to September 2022, we found that 71.9 per cent of members presented with more than one wellbeing issue, and nearly one in five people had five or more presenting conditions.
This meant that most people (who reached out for support) were contending with multiple, intertwined challenges, with the impact compounded for each challenge.
- To illustrate how varied those concerns were, our data shows that from January to September 2022, our clinical team (including registered nurses and specialist physicians) diagnosed more than 100 distinct medical diagnoses.
What does this mean?
It means a one-size-fits-all referral to an employer-funded psychologist isn’t always appropriate and/or isn’t always enough. The benefit of combining mental health support with medical (and safety) support allows an upfront triage by a qualified clinician, to avoid conditions being overlooked (or treated in the wrong order).
Why is employee wellbeing affecting business performance?
When employees are not well, their poor wellbeing typically presents in the workplace as absenteeism, presenteeism, emotional contagion, workers’ compensation claims, and/or resignation.
Each of these can prove costly (e.g. absenteeism costs the Australian economy $35+ billion annually in wages and lost productivity, presenteeism costs $34 billion, and the workers’ compensation paid for work-related mental health conditions was last reported at $904.9 million), and a risk to long-term organisational resilience.
References: Direct Health Solutions, Australian Broadcasting Commission, The Centre for International Economics, Medibank, Safe Work Australia (2022, National Dataset for Compensation-Based Statistics, custom data request)

Why should employers share responsibility for worker wellbeing?
Our next article in this series will explore the concept of shared responsibility for worker wellbeing, and include quotes from people leaders at some of Australia’s leading organisations.
To stay in the know, we invite you to follow us on LinkedIn and/or regularly check our articles.
About Sonder
Sonder is a technology company that helps organisations improve the wellbeing of their people so they perform at their best. Our mobile app provides immediate, 24/7 support from a team of safety, medical, and mental health professionals – plus onsite help for time-sensitive scenarios. Accredited by the Australian Council on Healthcare Standards (ACHS), our platform gives leaders the insights they need to act on tomorrow’s wellbeing challenges today.



