For years, support programs have prescribed the urgent deployment of a psychologist or trauma counsellor to the scene of a critical incident or traumatic event. As a result, well-intentioned universities keen to exercise their duty of care have traditionally agreed to pay for a psychologist to be sent on-site to support their students and staff after traumatic events.
What does the evidence say
Psychological debriefing may do more harm than good and most people should not need direct psychological support in the first instance.
Psychological debriefing (including critical incident stress debriefing to reconstruct the traumatic event) is not the best clinical practice. The evidence has for some time suggested that “psychological debriefing is ineffective and has adverse long-term effects. It is not an appropriate treatment for trauma victims,” said Mayou, Ehlers and Hobbs in the British Journal of Psychiatry, and Forbes et. al. in the Australian and New Zealand Journal of Psychiatry.
This sentiment was echoed in the World Health Organisation (WHO) literature review (2012) which concluded that “psychological debriefing should not be used for people exposed recently to a traumatic event as an intervention to reduce the risk of post-traumatic stress, anxiety or depressive symptoms”.
Several studies also show that psychological debriefing can make symptoms worse:
- A study of police found that those who had psychological debriefing exhibited more hyperarousal at follow-up than those who did not receive a debriefing;
- A study of road accident victims discovered that the intervention group had a “significantly worse outcome” at the three-year mark, “in terms of general psychiatric symptoms (BSI)#, travel anxiety when being a passenger, pain, physical problems, [the] overall level of functioning, and financial problems”;
- A burn trauma victims study showed 26 per cent had post-traumatic stress disorder (PTSD) at follow-up, compared to 9 per cent of the control group; and
- The Cochrane Review of 11 clinical trials found no evidence that psychological debriefing reduced the severity of PTSD, depression, anxiety and general psychological morbidity, and “some suggestion that it may increase the risk of PTSD and depression”. They recommended that “compulsory debriefing of victims of trauma should cease”.
#Brief Symptom Inventory

Psychological First Aid (PFA) is the modern approach to critical incidents and disasters. Its premise is that people are resilient and in most cases can recover naturally from trauma.
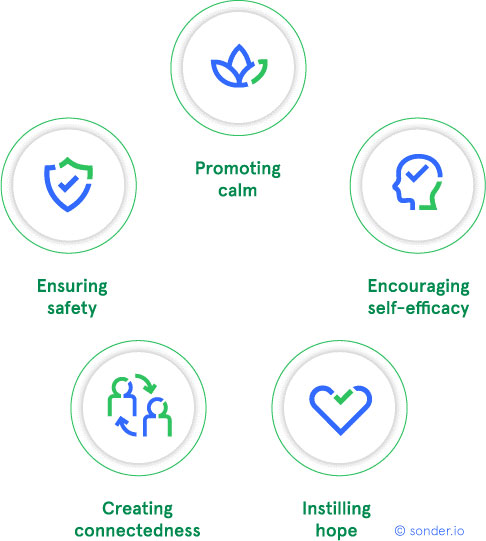
PFA is a “humane, supportive response to a fellow human being who is suffering and who may need support”, says the WHO. This involves helping people feel safe, connected to others, calm and hopeful, and ensuring access to physical, emotional and social support. It aims to reduce initial distress, meet current needs, promote flexible coping and encourage adjustment – and it can be delivered by peers, managers and colleagues.
“Most people recover naturally from trauma, without the need for formal mental health intervention. For individuals who might benefit from trauma support, this is best provided in a style, on a timeframe, and by a practitioner who best suits the needs of that individual,” says Sonder’s Dr Phillips.
Five principles of psychological first aid (PFA)
Summary
Six years after 25 Australian universities joined together to form the Australian Health Promoting Universities Network, and two years after COVID-19 re-elevated the importance of student and staff wellbeing, today’s university leaders and senate committees are prioritising institutional wellbeing.
Health-savvy university leaders understand that wellbeing affects: student success; Student Experience Survey results; student and staff retention; staff productivity; and as the International Labour Organization says, “an organisation’s long-term effectiveness”.
As part of this prioritisation of student and staff wellbeing, it’s important that institutions consider the evidence around psychological debriefing and the official recommendations to replace it with psychological first aid, in order to best protect their people and not inadvertently do more harm than good.

Want to learn more?
To read the other four myths about student and staff wellbeing, we invite you to download our evidence-based report, 5 myths about student and staff wellbeing.
For more information about how Sonder can help you rethink your university’s student and staff wellbeing strategies, we invite you to contact us here.
About Sonder
Sonder is a technology company that helps organisations improve the wellbeing of their people so they perform at their best. Our mobile app provides immediate, 24/7 support from a team of safety, medical, and mental health professionals – plus onsite help for time-sensitive scenarios. Accredited by the Australian Council on Healthcare Standards (ACHS), our platform gives leaders the insights they need to act on tomorrow’s wellbeing challenges today.



